The Stone Clinic Blog by Kevin R. Stone, MD
Sign up for Dr. Stone's weekly blog. Described as a "gift to his patients" this short, weekly column provides the latest expert insight on sports, performance, & orthopaedic care.
Dr. Stone's Latest Blogs
How to Run Forever on the "Rambling Runner Podcast" with Dr. Stone
Dr. Stone appeared this week on the Rambling...
Blog
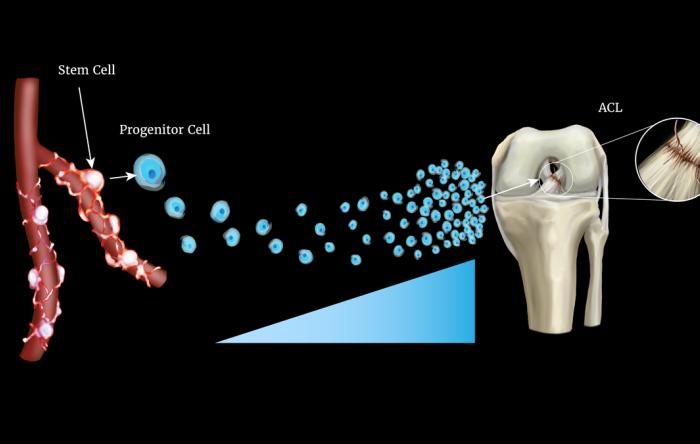
Is the ACL Crisis in Women’s Sports Solvable?
ACL ruptures are in the news during the 2023 FIFA...
Blog
Injured Your ACL? Take Care of Your Other Knee Ligaments Too
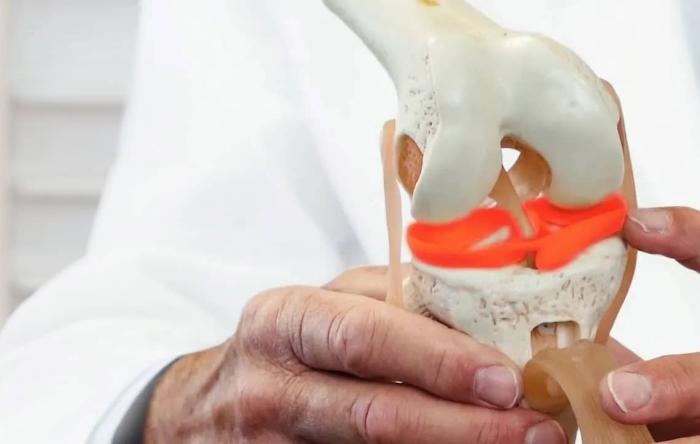
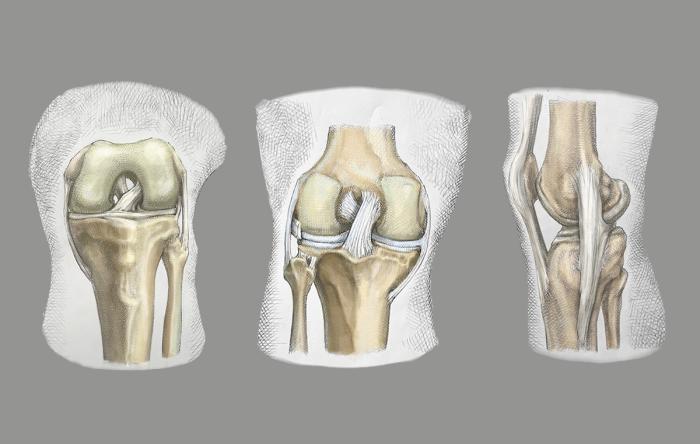
The knee is tied together by more than just the...
Blog
How to Repair Your Shoulder Without Surgery (VIDEO)
Most shoulder injuries can be repaired without...
Blog
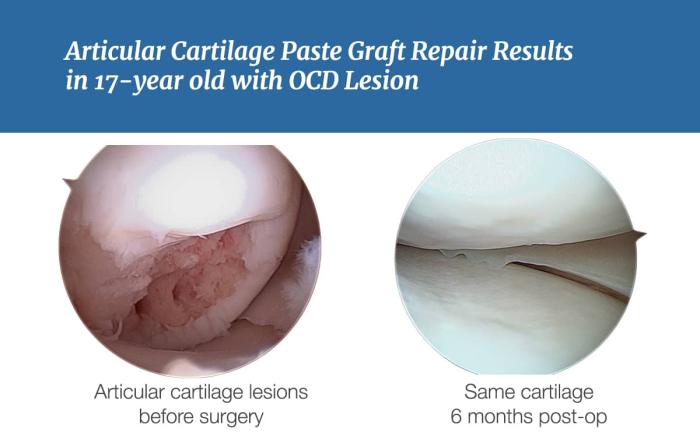
Paste Grafting and Stem Cell Cartilage Repair in 2023
Articular cartilage covers the ends of all bones...
Blog