No Meniscus Procedure Is Ever Standard
Hear From Our Patients
Skier avoids knee replacement with BioKneeA surgeon should never treat a meniscus repair as an assembly-line process. When I hear a patient say “The doctor told me it’s a standard procedure,” I often think that means there isn’t much thought being put into it. In my mind, there is no such thing as a “standard procedure.” Or a patient will tell me, “I was told I have a torn meniscus cartilage in my knee. The doctor said it’s simple to just remove the torn part. He does it all the time.”
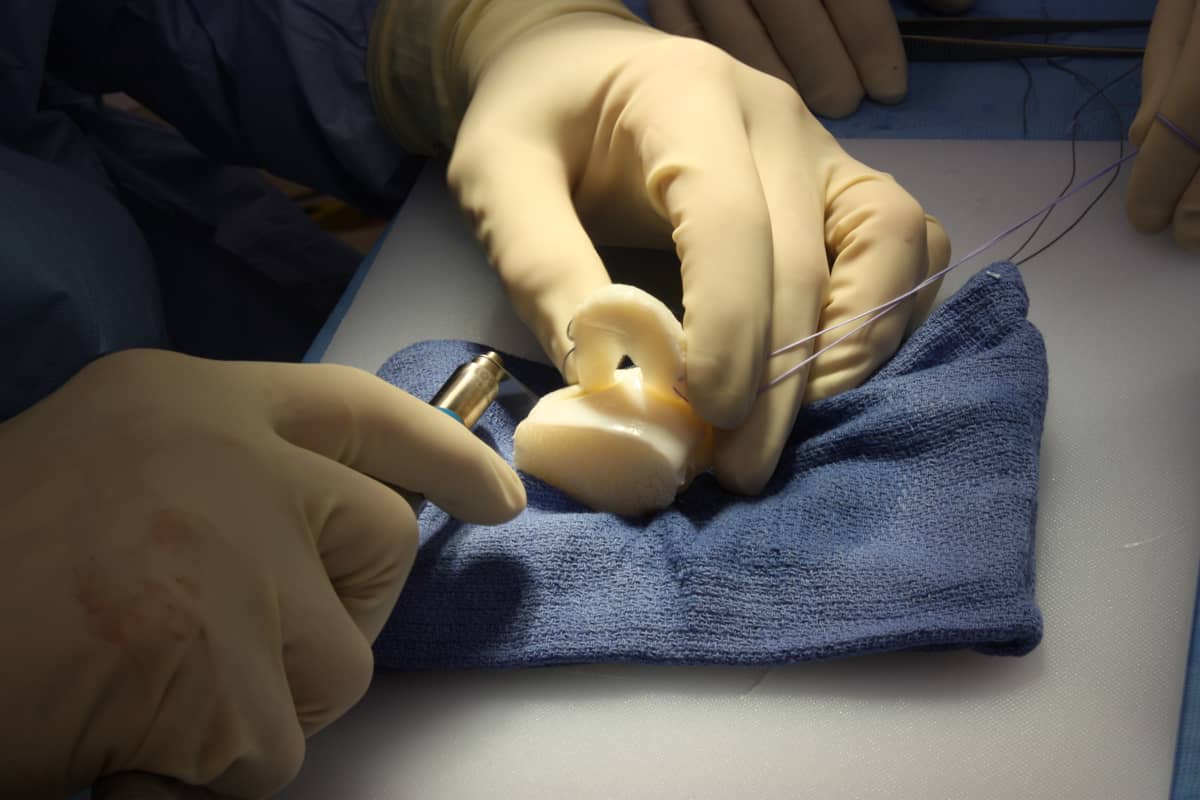
Ugh, I think. Actually, each person is different. Each knee is different. Each torn meniscus cartilage is different. And most importantly, the goals and outcome of each procedure are different. Let me explain.
The meniscus is the key shock absorber in the knee. When even small amounts of it are removed, the force concentration on the tibia goes up, wearing away the bearing surface and leading to early arthritis. When it’s torn, the goal is to save as much of the meniscus as possible, preferably by repairing it—or, if it’s truly irreparable, by removing as little as necessary to recreate a smooth surface from the frayed edges. Even the most common tears often have extra side tears or hidden degenerative areas that can affect the results.
The artistry of the surgeon determines how smooth and shaped the remaining tissue will be. The surgeon’s scientific understanding of how important the tissue is, how to stimulate a new blood supply, how to use injections of growth factors to augment healing, how to recruit stem-cell-derived progenitor cells to the site of healing, how to suture the torn edges, or (if necessary) how to replace the meniscus with a new donor meniscus, all pre-determine how the surgeon is going to act when faced with the unique tear inside your unique knee.
Your own preferences also contribute to making your case unique. Are you willing to have a longer rehab period in order to permit tissue healing? Are you okay if an effort to save your meniscus fails and you need a follow-up procedure? Do you just want to get back to work quickly and aren’t concerned with the long-term outcomes? Do you want to run marathons and need every bit of shock absorption possible? If a significant portion of the meniscus is fatally damaged, is the surgeon prepared to replace your meniscus during the same surgery? Have you and your surgeon agreed on the goals of the surgery?
I believe there is tremendous art to surgery and science to the artistry. I believe every patient and every problem—not just every meniscus injury—is unique, and that it’s important to try to match the surgeon’s skills with the patient’s needs. Part of a surgeon’s job is to educate patients not just about what we can do today, but about what the future is bringing in terms of new techniques and understanding. And I believe every surgeon should be thinking about—and working at—how to improve every surgical procedure.
So if you are told that your procedure is standard, remember to ask, “Whose standard?”
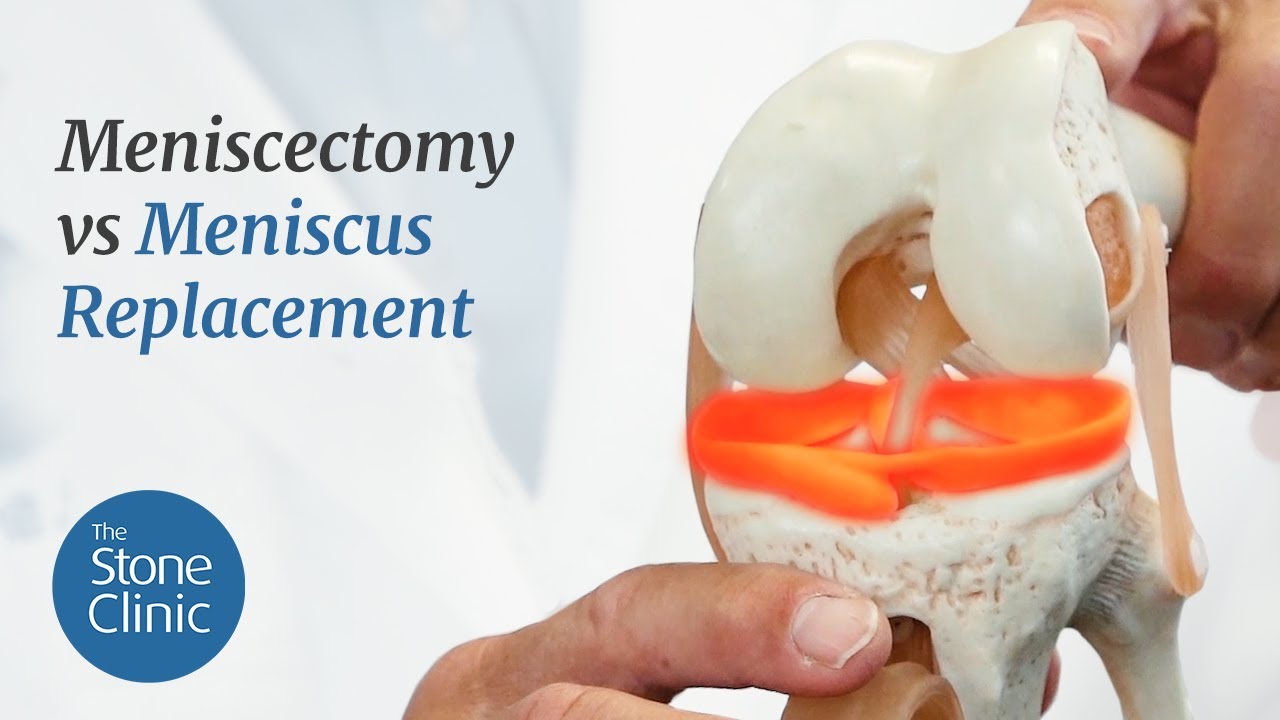
Meniscectomy vs Meniscus Replacement: Meniscus Tear Treatment Options
Kevin R. Stone, MD, is one of the world’s leading experts in meniscus transplantation and a pioneer of biologic orthopaedic techniques. For over 30 years, he and his team have specialized in giving people back their vital meniscus shock absorbers, keeping the knee moving naturally, and reducing the likelihood of a total knee replacement.