Injection Elixirs: How Four “Drugs” Have Changed Orthopaedics
Hear From Our Patients
Back to Sports After Ankle Injections & Physical TherapyAs an orthopaedic surgeon, I focus on surgical techniques to fix problems and rehabilitation exercises to help the patient become better than they were before they were injured. In addition to those two strategies, four “drugs” have dramatically changed my practice. Here they are:
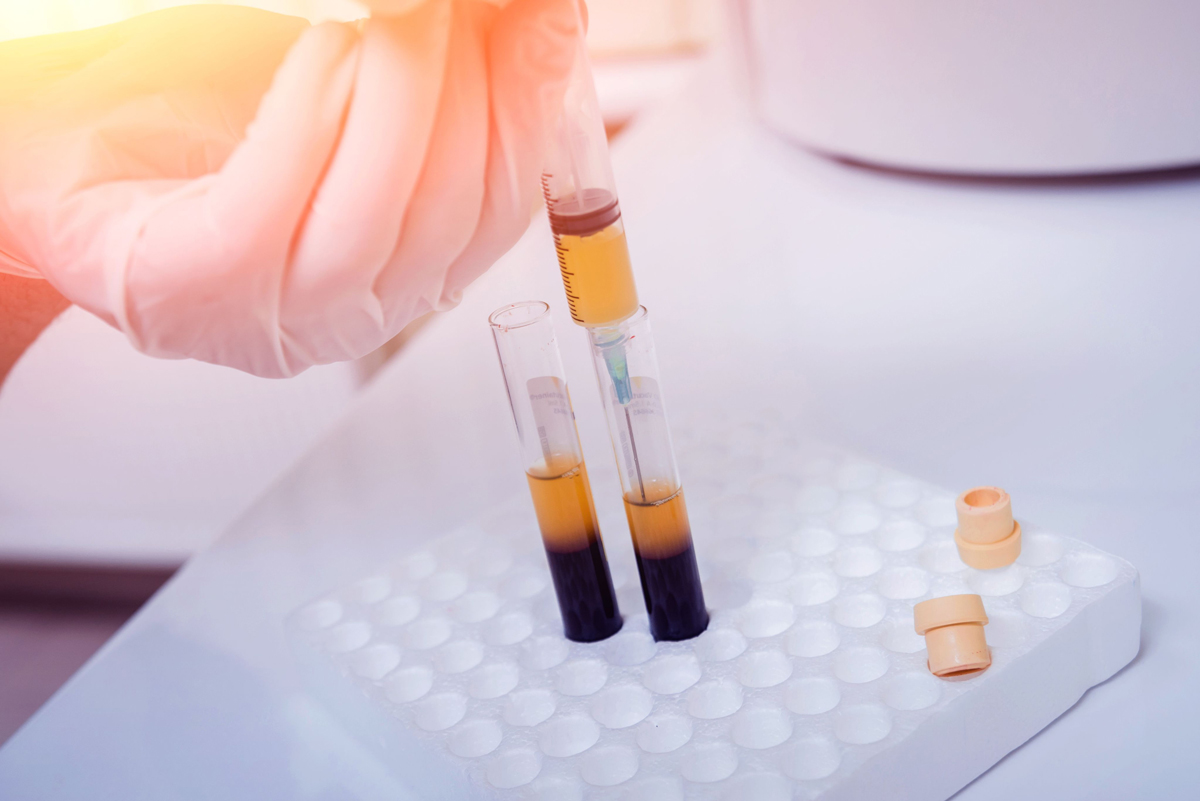
1) PRP: Platelet-rich plasma—primarily the growth factors and proteins concentrated from the platelets in the blood—is now recognized to be such a potent anti-inflammatory and pain reliever that it has become our first-line therapy for many orthopaedic injuries. Part of its remarkable mechanism of action includes increasing the synovial cell production of hyaluronic acid (the natural lubricant of the joint) and recruiting the body’s own billions of stem-cell-derived progenitor cells to the joint or site of injury. The effects are so profound that many of my severely arthritic patients—with knees that, in the past, would have needed a joint replacement —now come in each year, often before ski season, for their “joint lube cocktail” of PRP plus hyaluronic acid. And many of my degenerative torn rotator cuff patients do the same. They get an injection, work with our rehab team, and delay their shoulder surgery—often permanently.
PRP will be further improved by the addition of birth tissues from healthy c-sections, once the FDA approves them. They are rich sources of all the factors that growing or healing tissue needs and will likely dramatically improve the outcomes of all surgical and non-surgical repairs.
2) TXA: Tranexamic acid is a drug given just before surgery. It inhibits bleeding without increasing the risks of blood clots. It is an antifibrinolytic, meaning it inhibits the breakdown of the natural blood clot that forms at the bleeding vessel. It is so effective that we no longer use a tourniquet for any of our orthopaedic procedures—including total joints and fractures. By its mechanism of action, TXA also markedly reduces the post-op swelling. This effect reduces pain and complications and accelerates healing. It has speeded up surgery and is a godsend to both surgeon and patient.
3) Toradol (Ketorolac) and long-acting Marcaine/anti-inflammatory gels: Toradol is an inhibitor of prostaglandin and thereby provides significant pain relief combined with an anti-inflammatory aspect. New anesthetic gels that combine the “-caine” drugs with NSAID anti-inflammatory drugs are now available to bathe the tissues at the time of surgery. They are such potent pain relievers that our total joint patients use little or no narcotics post-surgery. By using Marcaine-like drugs before an incision, the patient’s brain never gets the pain signals during surgery and the anesthesiologist is thus able to use fewer sleeping drugs. When the gel combinations are applied to the open wounds at the end of surgery, the patient awakens with minimal to no pain at all. By using the combination of Tylenol and Toradol (T&T, as we call it) at the onset of any ache, patients are able to exercise with their therapists during the days immediately after surgery and work to regain full motion promptly. No pain means full gain today.
4) THC and CBD: While we cannot prescribe THC per Federal law, we recognize that many of our patients now turn to “gummies” for sleep during the post-op period. Our initial observations are that THC has reduced anxiety, improved sleep, substituted for pain medication, and helped the entire rehab process. I suspect its use will become more mainstream. Although we have no clear data and not enough experience with the use of CBD alone, we do not believe it provides the same level of relief for the patients as a THC/CBD combination. These combination formulations seem to provide for many happy patients—and happy patients make happy doctors.