Bowlegged: The Varus Knee
Hear From Our Patients
Marathon Running in his Seventies on a Total Knee ReplacementsEvery great runner is bowlegged. Something about the curve permits optimal push off and speed. The normal human population has leg angles that vary from zero to five degrees inward bowing (called varus) or outward knock-kneed (valgus). Unfortunately, this is not always an advantage.
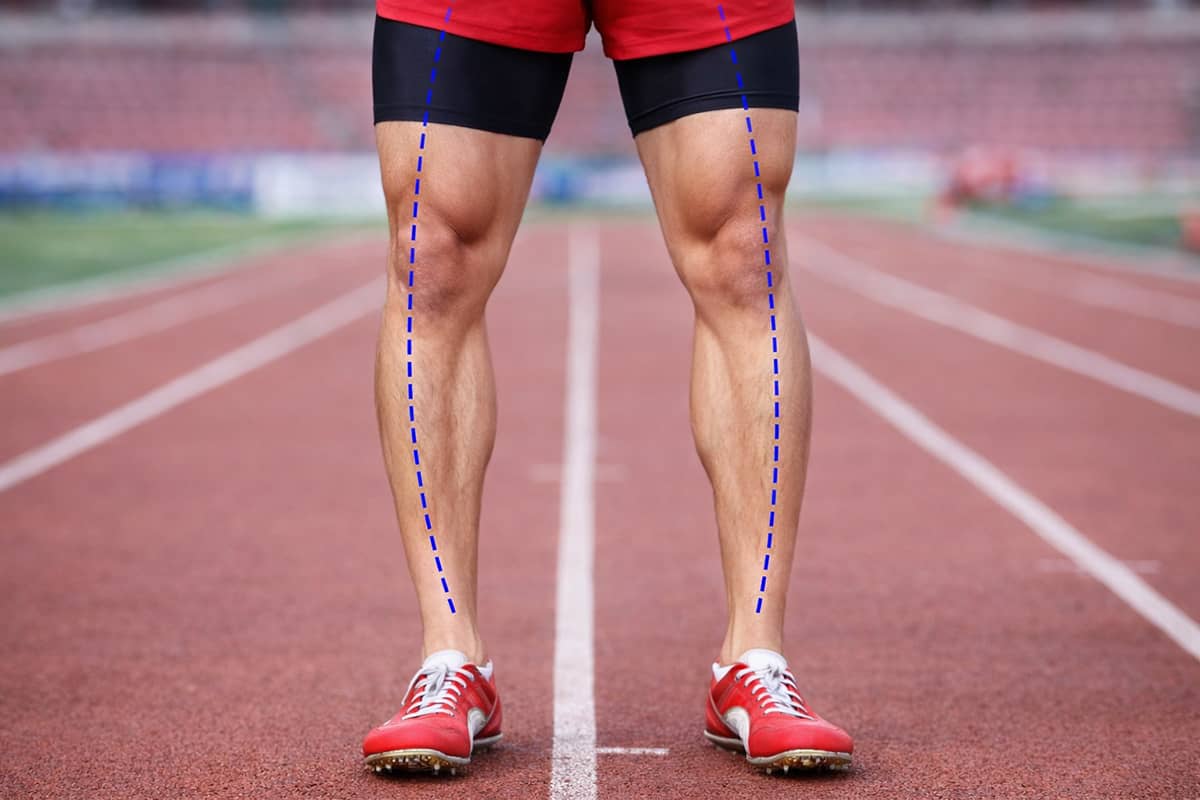
People are either relatively straight-legged, knock-kneed, or bowlegged. The forces in the joint when walking are not evenly distributed in the angled knee. Still, in healthy, uninjured legs, these variations exist happily for a lifetime. Unfortunately, if the knee joint is injured—such as a torn ACL, meniscus, or the articular cartilage bearing surface—the increased forces become a liability. This is especially true with men, as many males gradually become more bowed with aging, most likely due to loss of the articular cartilage and meniscus in the knee. Here are a few examples.
When a bowlegged person tears their meniscus cartilage, the forces of the femur on the tibia become concentrated in a smaller area on top of the tibia. Even a 20% loss of the posterior horn of the medial (inside meniscus) leads to a 160% increase in force in the newly exposed area. Since people walk two to three million steps per year at up to five times their normal body weight (depending on the height of the step or jump) an increase in force concentration quickly overloads the normal articular cartilage, exposing the underlying bone.
The same is true for the knock-kneed individual. Loss of the lateral meniscus quickly dooms the young athlete’s knee in all alignments, but in the knock-kneed person, the arthritis sets in especially quickly.
In both the bowed and knock-kneed, the curvatures become worse over time as the compartments narrow with loss of the articular cartilage.
So, what to do about it? The orthopaedic community is divided between those surgeons who believe in early osteotomy (cutting of the bones to align the knee in a straight angle) and biologic replacement surgeons like me, who believe the primary problem—and the one that should be addressed first—is the loss of cartilage.
The osteotomy surgeons make the case that bad biomechanics will kill good biology any day of the week. As only a relatively few of them are trained in meniscus replacement and cartilage regrowth procedures, they cut the bones first. Biologic replacement surgeons believe that the complications from osteotomy and the changing of the entire body’s gait by straightening the knee in patients who have lived a lifetime with curved bones is not a wise first step. We believe in replacing the meniscus and regrowing the cartilage first and only changing the alignment if it is more than seven degrees off straight, or if the biologic treatments are not adequately successful.
Occasionally, when the alignment is greater than seven degrees, we combine alignment surgery with biologic replacement.
Age, as many might initially think, is not necessarily a key factor. We published a 2- to 25-year outcomes study on meniscus replacement and cartilage repair in patients over 50 years of age who were told they needed an artificial joint due to loss of cartilage, pain, and narrowing in part of their knee. 42% of patients went on to partial or total knee replacement at an average of eight years. 48% never progressed to requiring an artificial joint.
A recent publication ( Lin E et al: AM J Sports Medicine 2026;65 (1):216-222) reported 1-10% of patients convert to an artificial knee joint within one year of a meniscectomy (removal of part of the meniscus) yet after a meniscus replacement, for those who converted to a total knee, the mean time was 10 years.
So, we celebrate the diversity of angles people present with. If only they wouldn’t get injured, we wouldn’t need to debate what to do for them.

