Knee Articular Cartilage Damage / Osteoarthritis: Diagnosis & Repair
For over 30 years, we have regenerated damaged articular cartilage to help people preserve their natural joints and avoid artificial replacement. Our cartilage repair technique, the articular cartilage paste graft, uses a patient’s biologic healing response to stimulate the regrowth of damaged cartilage surfaces, relieving articular cartilage pain and allowing patients to return to high-level sports—including running and impact sports.
What is Articular Cartilage?
Articular cartilage is the smooth, white tissue that covers the ends of bones within a joint. It facilitates smooth, pain-free motion and helps to absorb impact during activities like walking or running. Damage to this essential cartilage can lead to joint pain, inflammation, and loss of mobility.
Understanding Articular Cartilage Pain and Knee Cartilage Damage
Knee articular cartilage damage can result from various causes, including:
- Sports injuries or trauma
- Conditions like osteoarthritis or inflammatory arthritis
- Meniscus cartilage removal or prior joint injuries
Bone malalignment or excess weight increases pressure on the joints and also contributes to damage. Normal use, including running, won’t wear out the cartilage unless it’s been previously injured or if the meniscus cartilage has been removed in a previous surgery.
Once articular cartilage is damaged, it cannot heal on its own. Over time, untreated damage breaks down the cartilage and bone spurs form. This can lead to severe conditions like traumatic osteoarthritis where cartilage loss causes swelling, inflammation, and further joint degeneration.
If not treated, the cartilage wear will eventually progress to the point where the bones on each side of the joint come into direct contact, referred to as bone-on-bone wear. At this stage, artificial joint replacement becomes the only available option to address the injury.
Severity Grading for Articular Cartilage Damage:
- Grade 0: Normal, healthy cartilage.
- Grade 1: Cartilage has a soft spot or blisters.
- Grade 2: Minor tears visible in the cartilage.
- Grade 3: Lesions have deep crevices extending through more than 50% of the cartilage layer.
- Grade 4: Exposed underlying bone.
Our Long-Term Solution for Articular Cartilage Repair
Addressing knee cartilage damage early can dramatically improve long-term outcomes. Our biologic joint replacement techniques target knee cartilage damage before it reaches the bone-on-bone stage. Using a procedure pioneered by Dr. Stone called the Articular Cartilage Paste Graft, we repair and regenerate cartilage, reversing arthritic damage and preserving the knee joint. This solution has helped hundreds of our patients return to high-level sports—including running—and avoid/delay artificial knee replacement.
What is the Articular Cartilage Paste Graft Procedure?
In 1991, Dr. Stone developed the articular cartilage paste graft technique to address the critical need for a more effective cartilage repair method. It is a minimally invasive, one-step arthroscopic procedure that stimulates articular cartilage regeneration—even in arthritic joints.
During the procedure, the surgeon prepares the damaged area by creating a fresh blood supply and exposing marrow cells. A tissue graft is taken from a non-weight-bearing part of the knee, crushed into a paste, and applied to the damaged cartilage. As this area heals, healthy cartilage forms in its place.
Dr. Stone Describes the Articular Cartilage Paste Graft Procedure

"Articular cartilage paste grafting has provided my patients with tremendous relief and permitted a return to sports for many arthritic joints that were thought to require joint replacement. Our published peer reviewed long-term outcome studies have matched or exceeded any other published work. Paste grafting has been a great tool for salvaging failed microfractures and other cartilage procedures."
Clinically Proven Success of Our Cartilage Repair Approach
Backed by decades of peer-reviewed clinical research conducted by the Stone Research Foundation, independent clinical studies demonstrate that this repair technique generates healthy, durable cartilage tissue. A 10-23 year follow-up study confirmed that this procedure leads to:
- Long-term improvements in function - Average benefit time of 19 years1.
- Significant reduction in pain - 90 percent of patients reported that the procedure provided good to excellent pain relief1.
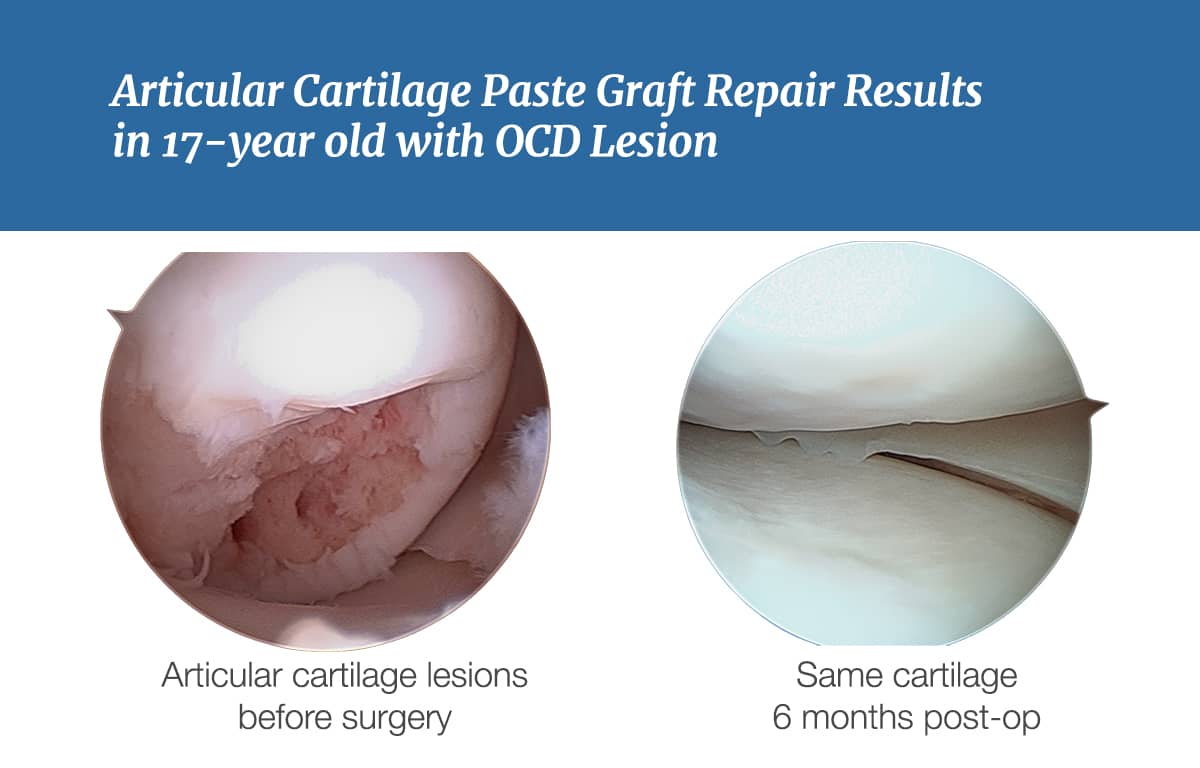
Our Knee Cartilage Repair Patient Outcome Stories
Be inspired by real patients who’ve undergone this procedure, reclaimed their lives, and returned to what they love—whether that’s pursuing high-level sports or enjoying everyday activities pain-free.
Partial or Total Knee Replacement at The Robotic Joint Center
When cartilage damage progresses to a bone-on-bone stage, biologic repair may no longer be viable. For patients with bone-on-bone wear in one or multiple compartments of their knee, we heal them and return them to sports using robotic knee replacement.
We have patients now running triathlons and (ultra)marathons, climbing mountains, skiing a hundred days a year on their replaced parts inside their knee. The groundbreaking innovations in robotic surgery are redefining the limits of our athletes and expanding the expectations of what is possible after knee replacement.
Take the First Step Toward Becoming Fitter, Faster, Stronger
Don’t let knee pain limit your life. Early diagnosis and treatment are key to preventing the onset of bone-on-bone arthritis and avoiding artificial knee replacement. Dr. Stone and our team of highly-trained physical therapists are here to guide you through your recovery with the goal of returning you to sports fitter, faster, and stronger than you've been in years. Book an appointment online or call us at (415) 563-3110 for an appointment.
Study Citation
1 - Stone KR, Pelsis JR, Na K, Walgenbach AW, Turek TJ. 2016. "Articular cartilage paste graft for severe osteochondral lesions of the knee: a 10- to 23-year follow-up study." Knee Surgery, Sports Traumatology, Arthroscopy.

