Can Arthritis be Cured?
Arthritis can be caused by trauma, inflammation, or genetics. In sports-related injuries, we most often see trauma-induced arthritis. But inflammation, from diseases such as rheumatoid and gouty arthritis, can play a role in this as well. Here is a short introduction to the body’s response to traumatic arthritis and possible cures.
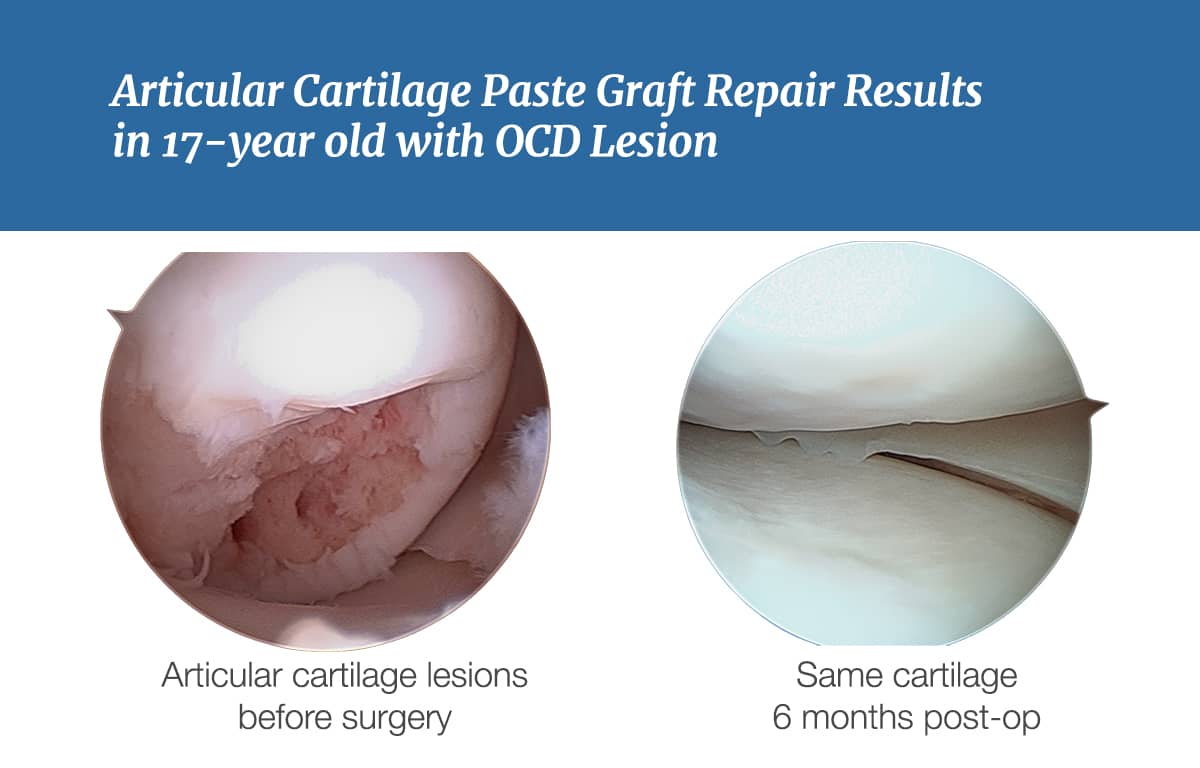
In a healthy joint, the bones are covered by articular cartilage on the white, shiny surface, as seen when you open a chicken wing. Five times as slick as ice on ice, with few cells and surrounded by a dense matrix of water and charged sugars, the cartilage often fails to heal after an injury. If the articular cartilage is damaged to the level of the underlying bone (but not into that layer), no healing occurs and the joint degrades with widening of the exposed bone.
However, when the injury involves the bone marrow below the cartilage—an area where the blood supply is abundant—pro-inflammatory white cells (neutrophils) are activated. They clear the injury site of damaged tissues and recruit repair cells called monocytes. Cytokines (proteins released from the white cells) activate these monocytes, shifting them to cells called macrophages. These macrophages remove the injured and dead cells, and present antigens to recruit the anti-inflammatory and pro-regenerative helper (T) cells.
This process initiates the pro-regenerative phase, during which the body’s own stem cells are stimulated to divide into “progenitor” cells. These cells rush to the site of injury, directing the healing response. Fortunately, humans have billions of these stem-derived progenitor cells, waiting on the walls of vessels to be called into action when an injury occurs.
Today, the trick—in medicine and surgery—is mobilizing this healing response to induce reformation of the articular cartilage surfaces before the underlying bone becomes deformed and diseased by loss of its protective cartilage cover.
This is why the field is moving away from treating joints with pain relievers, NSAIDS, or even injections of a few million cells, and towards using recruitment factors to stimulate the billions of cells awaiting the call.
The recruitment factors most commonly used are from the patients’ own platelets, derived from blood spun in a centrifuge and reinjected back into the damaged joint or tissue. While other sources, such as birth tissues from healthy C-sections (Wharton’s jelly, amniotic fluid, etc.) are the most potent sources of recruitment factors, they are currently on hold by the FDA. This is because the government has deemed them “drugs” rather than “devices,” therefore requiring extensive and expensive trials to be performed before they can be approved—a process that will take years.
Other drugs and supplements are focused on the removal of injured and dead cells, which elute the degradative enzymes that accelerate the erosion process. Early removal of dying cells has been shown to rejuvenate diseased tissue—and this may be a pathway to an arthritis cure. Mitochondria, the power plants of cells, also change with aging and disease and are the target of novel therapies. Though these drug therapies live mostly in the life-elongation space, they may come to play significant roles in the treatment of arthritis.
The other aspects of the development of post-traumatic joint arthritis are the loss of key protective tissues, joint stabilization, and joint mechanics. As the cartilage layer degrades, the joints become angulated, bowed, or “knock-kneed,” and loading forces increase. If the protective shock absorber of the meniscus is missing, arthritis advances very rapidly.
Doctors have different biases on how to treat this. Our strategy is to repair, regenerate, or replace any injured tissues as soon as possible—especially the meniscus, and ligaments in injured knee joints. Loss of even small amounts of the meniscus, and loss of the joint’s stability from ligament injury, leads to abnormal force transfer through the joint surfaces and progressive loss of articular cartilage. This loss of cartilage combined with progressive deformity of the joint dooms the joints.
We are in a new era of orthopaedic science where both the biology and the biomechanics of joints can be manipulated effectively to treat, prevent, and even cure arthritis. This is a powerful time in the treatment of our friends and patients– because while cancer may kill you, arthritis ruins your life.

