Biologic versus Bionic Knee Replacement
Hear From Our Patients
Skier avoids knee replacement with BioKneeKnee replacements are all the rage. With an aging population getting more exercise, having good knees is one key to living well for a long time. Fortunately, there are now good options for knee replacement.
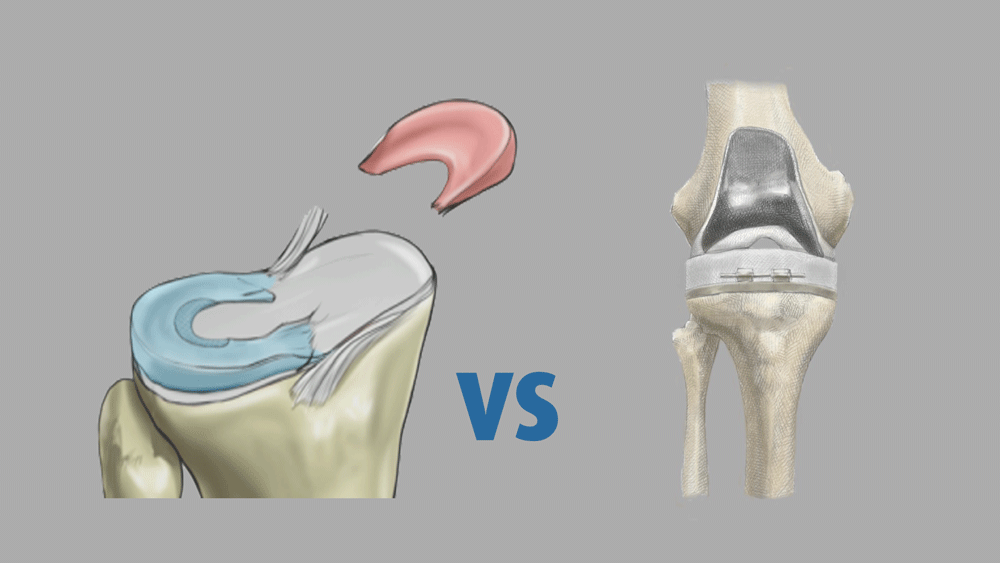
The knee joint bones are the kneecap (patella), the thigh bone (femur), and the shin bone (tibia). Each bone is covered by white, shiny articular cartilage, and protected by ligaments and meniscus fibrocartilage. Damage to the ligaments—such as an ACL rupture or a tear in the meniscus cartilage—leads to abnormal forces on the knee joint. These forces cause the articular cartilage-bearing surface to wear out. When the articular cartilage wears off down to the bone, you see early arthritis—which can progress to involve changes in the bones and the lining of the joint.
Biologic joint replacement is defined as restoration of the cartilage surface, usually combined with meniscus replacement and ligament reconstruction. These tissues are augmented with injections of growth factors to accelerate healing, and lubricated with injections of hyaluronic acid and growth factors to keep them healthy. Our clinic’s ongoing, 30-year study of articular cartilage paste grafting, combined with meniscus transplantation in arthritic knees, yielded improvement in pain and function for 80% of patients at the 17-year follow-up point (the longer data will be reported later this year). For most people in the 40- to 70-year age range, gaining a couple of decades of sports on biologically replaced knees is a much better option than living with pain.
Osteoarthritis affects 654.1 million individuals globally (1) leading to 2.6 million artificial knee replacements annually. (2) Still, many people have been told to wait for years before having their knee joint replaced, leaving them in pain—often with a limp and limited ranged of motion. The joint injections and drugs mentioned above help but do not affect the course of the disease. Artificial knee joints, on the other hand, when placed with robotic accuracy and without the use of cement, have evolved to permit a return to full sports. Why no cement? Because the newer components permit the bone to grow directly into the uniquely designed undersurface of the metal. Once fused to the bone, the likelihood of these implants coming loose is low. Increasing the exercise level of the patients causes their own bone to harden and their muscles to strengthen, further protecting the implants. So, departing from traditional wisdom, we encourage our patients to increase rather than decrease their exercise.
To summarize: Artificial joint replacement patients can return to full sports as long as their joint is placed perfectly, without bone cement, and their recovery includes a rehabilitation program focusing on immediate exercise to regain motion and power. While no promises can ever be made, it is far better to strive for an active athletic lifestyle than to rot in arthritic captivity.
Looking for more guidance on knee surgery? Check out Dr. Stone's article with key questions to ask during an office visit regarding knee surgery: Is Total Knee Replacement Right for Me?
Citation:
- Cui A, Li H, Wang D, Zhong J, Chen Y, Lu H. Global, regional prevalence, incidence and risk factors of knee osteoarthritis in population-based studies. EClinicalMedicine. 2020;29:100587. doi:10.1016./j.eclinm.2020.100587
- https://orthospinenews.com/2019/06/04/demand-for-knee-replacement-grows…
How to Avoid a Total Knee Replacement with a BioKnee
Our BioKnee® program biologically reconstructs the knee joint without the use of artificial implants. Head here to learn about our alternative to knee replacement.



