Why Microfracture Fails
Hear From Our Patients
Teenage Patient Overcomes Arthritis with Innovative Cartilage Repair SurgeryMicrofracture is a surgical technique used to repair damaged articular cartilage by making multiple small holes in the surface of the joint, which stimulates a healing response. The technique was frequently used in athletes after they injured their joints. Short-term results looked promising, though the results often deteriorated over time. Why is this?
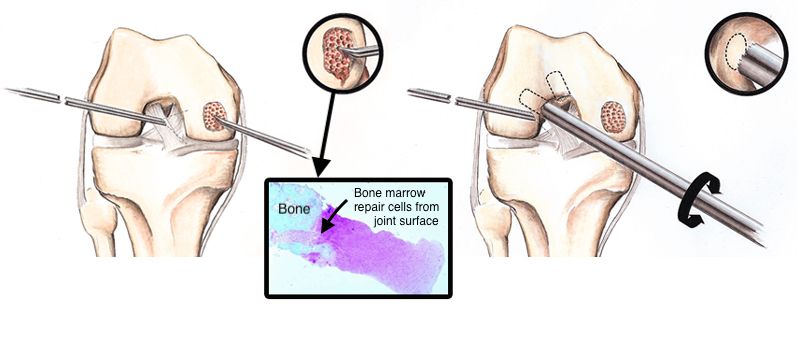
How Cartilage Injuries Progress to Arthritis
The surface of joints is covered with articular cartilage—a smooth bearing surface with a dense matrix, few cells, and no blood vessels. When injured by a fall or a sports injury, the dent in the articular cartilage never heals. If the injury is large enough to both expose the underlying bone and cause bleeding, a degree of healing can occur. But the repair tissue is usually not the same as the normal cartilage. When the healing is inadequate, pain recurs.
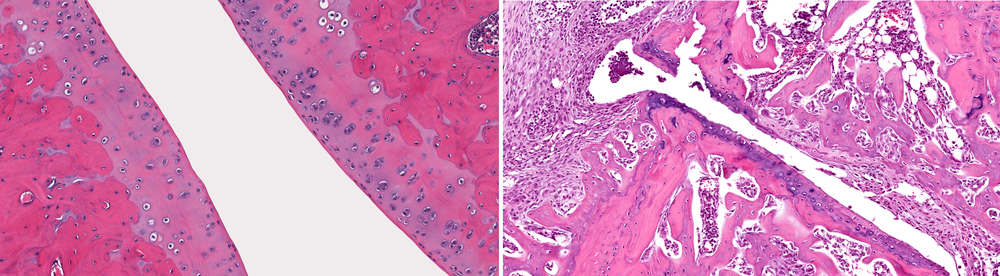
[Microscopic view of normal healthy joint (left) when compared to joint with osteoarthritis with loss of articular cartilage, fibrosis, inflammation and loss of bone (right)]
Over time, in the absence of healing, the initial damage to the articular cartilage gets worse. This leads to post-traumatic arthritis, a loss of cartilage, and the deformation of the underlying bone. This explains the intense efforts by surgeons to repair these cartilage lesions before they become a bigger problem. Repair methods range from non-operative injections of lubrication and growth factors to surgical interventions. These might include microfracture, cartilage plugs, cells grown in culture, matrices loaded with cells, articular cartilage paste grafting, or complete cartilage shell graft replacement.
These restorative techniques are trying to turn a degradative situation—where the cartilage is going to wear down—into an anabolic environment where the cartilage is stimulated to regrow or repair.
Does Microfracture Work? Success Rates and Why It Often Fails
Microfracture, by making holes in the underlying bone, brings a new blood supply to the surface. This blood supply carries the marrow progenitor cells. The clot that forms on the top of the bone at the site of the cartilage injury must heal and mature into an effective repair tissue for the procedure to work. Though the clot often does form, it has a varying ability to form into adequate cartilage repair material. The data from multiple studies in athletes [i],[ii],[iii],[iv],[v] shows that the repaired tissue breaks down over a few years, leaving exposed bone and causing more pain. Microfracture fails because the body loses the race between durable healing and repeated injury from weight-bearing.
Watch a brief explanation by Dr. Stone about why microfracture fails
Advanced Alternatives to Microfracture for Cartilage Repair
For cartilage repair to work consistently, it must be augmented. The healing tissue must be stimulated to form cartilage rapidly and durably. Our bias is to do this by adding progenitor/stem-derived repair cells, bone, and articular cartilage paste to a super microfracture (or morselization) of the lesion. This technique is called articular cartilage paste grafting. We augment that healing process by injections of growth factors from PRP, adding hyaluronic acid lubrication injections during the healing period. Other investigators are using variations of cells and growth factors in resorbable regeneration templates. Still others are testing new materials as cartilage replacements.[vi]
Each year, in normal walking, you take somewhere between two to three million steps. Each creates downward forces of up to five times your body weight, depending on the height of the step—never mind the torque and stress of pivoting. When microfracture fails, it is because natural healing alone is simply not effective often enough for a surface that sees so much force. Fortunately, the field is advancing fast enough so that the injuries we see today are likely to receive treatments designed to permanently repair the damage.
This reminds us that post-traumatic arthritis is preventable, treatable, and may even be curable. Now, if we could only avoid doing the damage in the first place…
-
To learn about how we treat the failures of the microfracture procedure, you may read Dr. Stone's article Failed Microfracture.
Article originally published Feb 2, 2015 and updated July 19, 2020.
Sources
[i] Goyal, D., Keyhani, S., Lee, E. H., & Hui, J. H. P. (2013). Evidence-Based Status of Microfracture Technique: A Systematic Review of Level I and II Studies. Arthroscopy : The Journal of Arthroscopic & Related Surgery : Official Publication of the Arthroscopy Association of North America and the International Arthroscopy Association, 29(9), 1579–88. doi:10.1016/j.arthro.2013.05.027
[ii] Gobbi, A., Karnatzikos, G., & Kumar, A. (2014). Long-term results after microfracture treatment for full-thickness knee chondral lesions in athletes. Knee Surgery, Sports Traumatology, Arthroscopy : Official Journal of the ESSKA, 22(9), 1986–96. doi:10.1007/s00167-013-2676-8
[iii] Gudas, R., Stankevicius, E., Monastyreckiene, E., Pranys, D., & Kalesinskas, R. J. (2006). Osteochondral autologous transplantation versus microfracture for the treatment of articular cartilage defects in the knee joint in athletes. Knee Surg Sports Traumatol Arthrosc, 14(9), 834–842. doi:10.1007/s00167-006-0067-0
[iv] Harnly, H. W., Krych, A. J., Rodeo, S. A., & Williams 3rd, R. J. (2012). Activity Levels Are Higher After Osteochondral Autograft Transfer Mosaicplasty Than After Microfracture for Articular Cartilage Defects of the Knee: A Retrospective Comparative Study. The Journal of Bone and Joint Surgery (American), 94(11), 971. doi:10.2106/jbjs.k.00815
[v] Gobbi, A., Nunag, P., & Malinowski, K. (2005). Treatment of full thickness chondral lesions of the knee with microfracture in a group of athletes. Knee Surgery, Sports Traumatology, Arthroscopy : Official Journal of the ESSKA, 13(3), 213–21. doi:10.1007/s00167-004-0499-3
[vi] De Coninck, T., Huysse, W., Willemot, L., Verdonk, R., Verstraete, K., & Verdonk, P. (2013). Two-year follow-up study on clinical and radiological outcomes of polyurethane meniscal scaffolds. The American Journal of Sports Medicine, 41(1), 64–72. doi:10.1177/0363546512463344
Dr. Stone Explains Our Long-Lasting Solution to Cartilage Regeneration
Dr. Stone explains how he regenerates damaged articular cartilage using a specialized technique he developed to help people preserve their natural joints and avoid artificial replacement