Failed Microfracture
Microfracture—the surgical procedure during which small holes are made in joint bones—has resulted in successful temporary repairs for thousands of injured athletes. Unfortunately, the repaired tissues often wore out—leading to more joint pain.
Fortunately, the science of cartilage repair today has better solutions. The failures of the past can now often be turned into athletic successes. Here is why.
Articular cartilage is the bearing surface of all joints. White, shiny, and smooth, it has a coefficient of friction five times a slick as ice on ice. This is due in part to its structure, to the lubrication fluid and proteins coating it, and to its ability to absorb and release water from charged carbohydrates in its matrix (a network of large molecules that provide support to the surrounding cells).
Once thought to be relatively inert, we now know otherwise. Not only does the articular cartilage have its own stem-derived repair cells; it can respond to injury with a rapid increase in the production of its own extracellular matrix. Simply put, articular cartilage tries hard to fix itself when injured.
When the cartilage is injured or knocked loose from the underlying bone by injury or disease, regeneration is possible—though not without assistance.
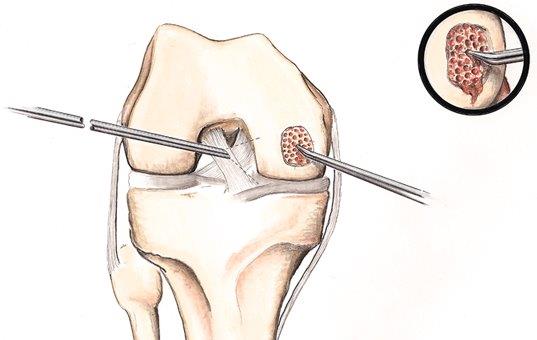
The first step is to massively stimulate a new blood supply by fracturing all the underlying bone (morselization, not microfracture), thereby releasing progenitor cells derived from marrow cells. These can induce a type of fibrous repair, similar to the way bone heals itself after injury.
The second step is to add a stimulating matrix to the marrow cells. The matrix we prefer is one made of articular cartilage and underlying bone, harvested from the notch of the knee and impacted into a paste. The paste matrix has all the signaling factors needed to tell the marrow cells to form normal articular cartilage.
Another type of matrix repair, called MACI, has recently been approved by the FDA for use in cartilage defects. Many of the same principles apply. These include exposing the marrow and providing a stimulating environment to induce cartilage repair.
The third step is to augment the repair with bioactive growth factors and lubricating injections from PRP and hyaluronic acid. The data is clear: These factors recruit the body’s own reparative cells (called stem cell-derived cells, or MSCs) to the site of injury. This accelerates healing and, most likely, solves the problems that microfracture alone could not.
The microfracture failures and joint pain that so many people live with are no longer a curse. The pain is a siren call: Get thee to a physician, and never let a treatment of the past define your future.