Fusion: The Failure of Science
Hear From Our Patients
Patient Avoids Ankle Fusion and Achieves Dream CareerFusing a joint in a human body is sometimes necessary to relieve pain. However, it is the last step in any treatment and represents a failure of either biology or science to create a cure.
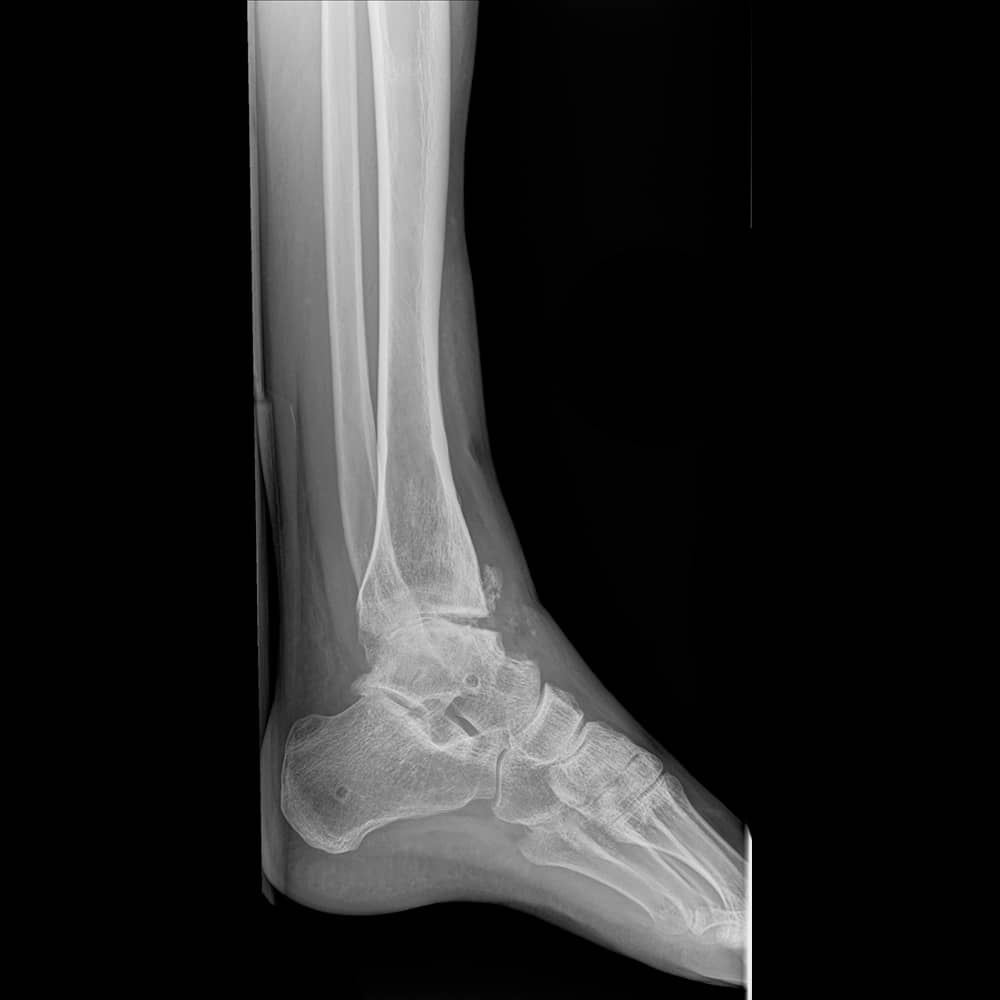
Ankle with near fusion
Many joints in the body get fused. The great toe, the ankle, the bones beneath the ankle (called the subtalar joint), the knee, the hip or shoulder (rarely), bones in the wrist, the elbow, and, most commonly, the vertebral bodies of the spine. Generally, what has happened is that an injury or arthritis led to the joint becoming diseased. Efforts to treat the joint with injections or surgical interventions failed, leaving the patient with ongoing pain. The last resort of fusion was then selected, accepting that compromised motion and function were a better alternative to pain.
Each fusion requires stripping away the remaining cartilage covering the bones, then screwing together the bones to compress them while the body heals by adhering one raw bone to another. Here are a few examples of joint degradation and thoughts about how we might approach them in the near future.
The great toe joint develops bone spurs after trauma (and yes, years of wearing high heels is considered trauma). This is because once the articular cartilage converting the joint surfaces is damaged, it does not heal without assistance. The damaged cartilage exposes the underlying bone to friction it is not designed to bear. Degradative enzymes and responsive growth factors are released by the lining of the joint (called the synovium), causing swelling and pain and the growth of bone spurs called osteophytes. Though the role of the spurs is debated, one function is to distribute the forces inside the joint more widely. The combination of spurs, swelling, and pain leads to loss of motion and exacerbates the biomechanical and biochemical causes of joint degeneration.
Classic surgical interventions often start with simple excision of the bone spurs and physical therapy to stretch out the scarred and tightened capsule of the joint. More severe cases are traditionally offered an artificial joint resurfacing or a fusion.
Injections of cocktails of other growth factors, immune-modulating proteins (cytokines), and lubricating factors are rapidly replacing cortisone injections. Cortisone reduces the pain for a short time, but further damages the joint by shutting down cellular metabolism and weakening the surrounding tissues. The biologic “cocktails” are being refined to provide both symptom relief and eventual disease modification by inducing augmented tissue repair after cartilage-grafting procedures restore the articular cartilage surfaces. And the cartilage-grafting procedures to either regrow or replace the damaged surfaces are improving rapidly.
None of these advances can be applied to a fused joint unless the fusion is surgically deconstructed (difficult, but not impossible). The other problem with fusion is that the mechanics of walking with a fused toe are so abnormal that the forces are directed into the midfoot, eventually causing joint degradation and pain.
The exact same problems arise in the other fusions. The forces are sent to the joints above and below…most commonly we see that while spine fusions provide relief at one level, a few years later they cause pain at the levels above or below.
What is clear is that fusion should be avoided whenever possible. The biologic options of cartilage repair and joint lubrication should be pushed past the known limits to maintain motion while limiting pain. Artificial joint replacements—including spine disc replacements—must be improved, so that return to full sports and activities are the goal and not the exception. And the desperate last resort of fusion will once and for all be abandoned.
A Patient's Story on Avoiding Ankle Fusion
Our patient David traveled to The Stone Clinic determined to avoid ankle fusion. Dr. Stone successfully repaired the dead bone and cartilage in David's ankle without the use of implants or hardware using a cartilage regeneration surgical procedure that he personally developed: the articular cartilage paste graft. You may learn more about David's story and BioAnkle treatment program here.
Ankle Replacement or Ankle Fusion. Which to Choose?
Our answer is: Neither! Patients told they need an ankle fusion or replacement, have more options. Advances in biologic therapies—including biologic ankle repair or injections of growth factors and joint lubrication—offer promising alternatives to people with severe ankle arthritis. Our BioAnkle program surgically treats arthritic ankles without hardware or implants, expanding the possibilities beyond invasive, end-stage procedures like fusion or replacement.