Artificial Meniscus Replacement
The meniscus is the natural fibrous cartilage that, by absorbing and distributing the normal forces of weight-bearing, protects joints from wear and tear. Here is the scoop on the efforts to replace this essential structure with artificial materials.
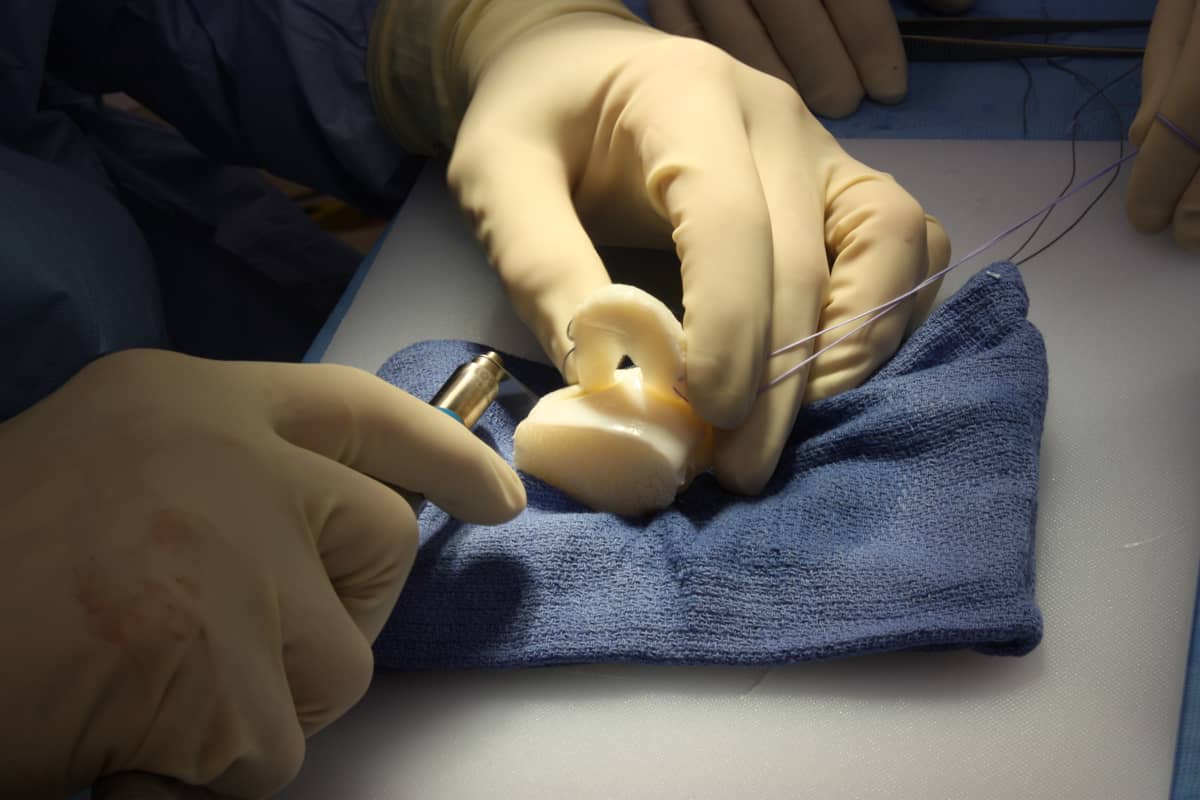
Dr. Stone preparing a human donor meniscus allograft for implantation.
The knee joint is a remarkable invention. With normal walking, the joint bears loads of up to five times our body weight, two to three million times each year. The matrix of the articular cartilage is also a marvel. Thanks to the interaction of water, the lubricant hyaluronic acid, and charged sugars called proteoglycans, the movement of the joint is five times slicker than ice on ice. Any artificial material inserted between the bones must be soft enough to not damage the pristine articular cartilage, yet durable enough to not flatten into a pancake under all of that force. No material known to mankind has enough softness, slickness, and durability to replace the natural meniscus.
But we continue to try. A newly approved urethane material called NuSurface, strengthened by Dynema (super-strong fibers), is the most recent entry into the field. Used just a few hundred times, it has provided pain relief to a select group of patients.
The patients must not have arthritis, as arthritis presents frayed articular cartilage surfaces or exposed bone. Either of these factors would, due to abrasion, dramatically increase the wear on the implant, and the device would quickly fail. The alignment and stability of these patients’ joints must be normal or correctable, and they must accept a limited return to impact sports.
What is great about the procedure is that it provides a solution for some patients. What is not so great is that the vast majority of patients who need a new meniscus fall into one of two categories. Either they are young, and want a natural tissue (such as a donor meniscus allograft, pictured above) that will permit a full return to sports; or they are older, suffer from arthritis, and seek pain relief in an effort to delay an artificial joint replacement. Neither group qualifies for the new artificial material. And if the patient has a healthy joint with smooth articular cartilage, why put in an artificial meniscus when a donor allograft meniscus is available?
The argument for the qualifying patients—those with limited athletic goals and healthy cartilage —is that the procedure using NuSurface is much easier for the surgeon, with an easier recovery period for the patient. Patients with limited ability to use crutches or participate in a careful rehabilitation program prefer this quicker approach.
The dream, of course, is to produce an artificial material with all the characteristics of a normal meniscus: the ability to absorb force, provide stability, and protect the joint. For now, the best material lives in people and animals.
The difficulties in using natural human tissues are that the supply is limited, the surgical technique is tricky, and rehabilitation takes time. The limited supply of young, healthy meniscus tissue could be solved if everyone were to choose to be donors upon death—or if people had to opt out of donation, rather than opt in. Most people would likely not bother to opt out, which would go a long way toward eliminating the shortage of tissue.
The supply problem can also be addressed by the use of animal tissues. The major problem with these transplants is rejection, as animals have a specific cell-membrane-based sugar that humans lack—and so human bodies reject animal tissues. We have recently demonstrated, however, that these animal sugars can be enzymatically removed before transplantation, essentially “humanizing” the tissues. Porcine tissue will be the first to be used, once it is tested and approved by the FDA.
The surgical technique is difficult and only a few centers in the world do a large volume of meniscus transplants. But with time and training, this will improve. The rehabilitation programs have also accelerated, as we now have better suturing and anchoring techniques—and we are able to add growth factors and lubricants, which diminish post-operative swelling and stiffness.
In general, working in concert with evolution and nature succeeds most often. Still, there is no end to our desire to do nature one better. Somewhere out there, at some point, we will find an artificial material that looks and acts like us.