Osteochrondritis Dissecans
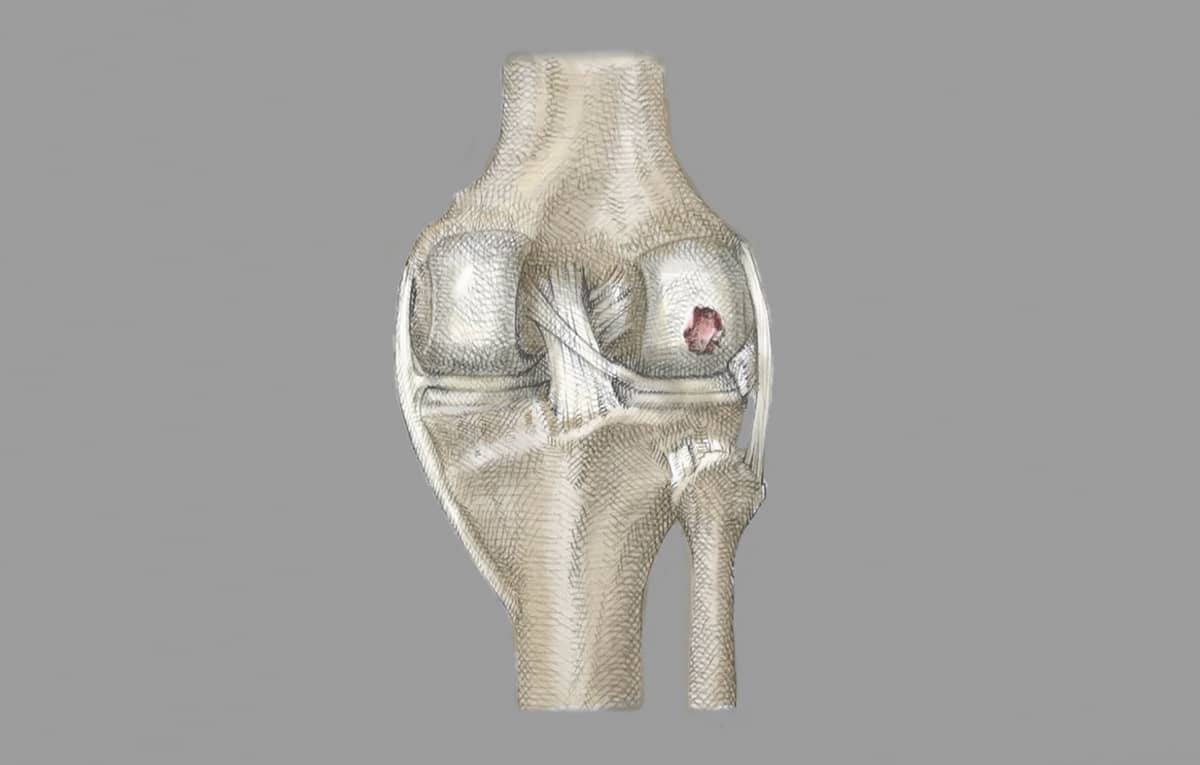
Osteochondritis Dissecans (OCD) is a disease in which localized osteocartilaginous separation at the level of the subchondral bone causes damage to the protective articular cartilage cover, subsequently producing pain and swelling.
Unless the lesion repairs spontaneously or it is treated, the disease process progresses. The affected area of subchondral bone and its attached articular cartilage can become loose and separate into the joint. In fact, this is a common source of loose bodies in the knee joint. OCD lesions may occur in any joint but are most common in the knee. OCD is most common in people between the ages of 10 - 50 years old, with more men being afflicted than women.
To repair OCD lesions, we applied our Arthroscopic Articular Cartilage Paste Grafting technique that has been used by Dr. Stone for the past 25 years to treat arthritic and traumatic lesions of the knee in over 600 cases with excellent pain relief. A study of the 2-12-year outcomes of Articular Cartilage Paste Grafting to treat arthritic lesions was published and can be found here. The goal in treating arthritic lesions, traumatic lesions, and failed OCD lesions with Articular Cartilage Paste Grafting is the same. The intent is to stimulate a healing response that covers the lesion with a protective layer of fibrocartilage and/or hyaline cartilage. The regenerated cartilage protects the underlying bone and serves to reduce pain and swelling. Articular Cartilage Paste Grafting has been successfully applied to OCD lesions as both a primary treatment and as a salvage procedure for defects that fail other attempts at repair.
The aim of this 2-13 year (7-year average) follow-up study was to evaluate seven consecutive patients undergoing osteochondral grafting of a failed OCD repair. The study found the following:
- Patients benefitted from significant improvements in pain, function, and activity scores
- 71% of patients had complete cartilage fill and full integration with the surrounding tissue
- No definitive correlation between clinical outcomes and MRI scores was observed

