Bone Bruises
Bones, like soft tissue, get bruised. The depressing difference is that sometimes these bruises are the first, middle, or last step in the development of arthritis. The old thinking was to just let them heal. The new thinking tells us to treat both the bruise and the cause of it before it gets worse. Here is how.
Bones are composed of an outer shell called the cortex and marrow on the inside. Unlike any other tissue in the body, a broken bone usually heals back to its normal bony architecture. This process is directed by unique cells called osteoclasts (which remove the damaged bone) and osteoblasts (which lay down the new bone). At the places where bones come together in joints, the bone ends are covered by a remarkably smooth tissue called articular cartilage. You see this white, shiny surface in chicken wings, or at the ends of the drumstick on the Thanksgiving turkey.
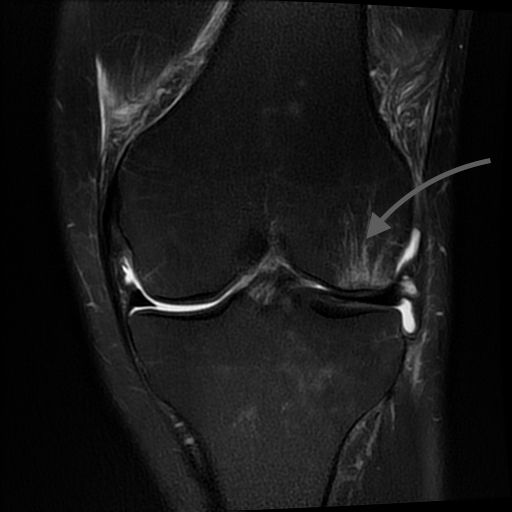
When an impact to a joint is strong enough to damage the articular cartilage (after a hard landing from a jump for instance), the underlying bone is also sometimes damaged. Or when the soft tissue shock absorbers in joints —the meniscus cartilage in the knee joint, for example—are torn or removed, the forces on the articular cartilage are concentrated in a narrow area and the underlying bone can be damaged over time. On an MRI, this damage shows up as a bone bruise. It is currently believed to be a pain generator in joints that hurt and a precursor to the progressive joint collapse we see in chronic osteoarthritis.
The question of whether or not bone bruises can be directly treated—and if this results in pain relief and prevents progressive joint disease—is a hot research topic right now. Current treatments for bone bruises are focused in several areas.
Non-operative care involves the use of bone stimulators, ultrasound, magnets, and electrical currents. The idea is to stimulate the osteoblast cells to produce more calcium at the site of the bruise. Whether or not direct intervention is undertaken, the first line of treatment may include loader braces, heel wedges (combined with gait training), weight loss, and muscle strengthening. No dietary supplements have been found to be helpful—yet. But some drugs used for hypertension and other medical conditions have been found to affect bony healing and are now in testing.
Direct interventions in the treatment of bone bruises involve injections of growth factors from bone marrow aspirate, fat, and other sources, combined with flowable calcium pastes, into the bony bruise. Pain relief has been noted in many of these patients. This is similar to the spine treatments (called kyphoplasty) that were provided for older people with collapse of the vertebral bodies. In those cases, artificial materials such as cement were used. Today, in younger, more active people, the goal is to actually stimulate healing and not just provide artificial support. Injectable growth factors not only have a direct effect on the osteoblasts, but they also recruit more of the body’s own stem-cell-derived self-repair cells to the site of injury.
But if the bone bruise alone is treated, and not its cause, arthritis is more likely to occur. So in joints where bone bruises occur due to loss of the articular cartilage surface, the ligaments, or the meniscus, the focus is now is to repair, regenerate, and replace these tissues. This should happen immediately upon loss, combined with bone bruise therapy. Excellent long-term studies have demonstrated the success of meniscus transplantation in early and late arthritis. We see similar results in articular cartilage repair using our paste technique, as well as with the cartilage replacement techniques developed by others, along with the benefits of ligament stabilization.
Isolated bone bruises are a different beast than those seen with joint damage and can be cured by a number of treatments. But if we are going to prevent, treat, and eventually cure the chronic osteoarthritis suffered by 9.3 million people in the U.S., bone bruise therapy—in combination with addressing its causes—is the path forward.
