Here’s a new joint. Now go home.
Total knee joint replacement has become a day surgery procedure. This is the most remarkable change in orthopedic care in the last decade. What was once a week-long hospital stay—accompanied by terrible pain, narcotics, surgical drains, urinary catheters, intravenous medication pumps, passive motion machines and significant complications—is now one night at home, and a visit to the therapist the next day.
How did this happen?
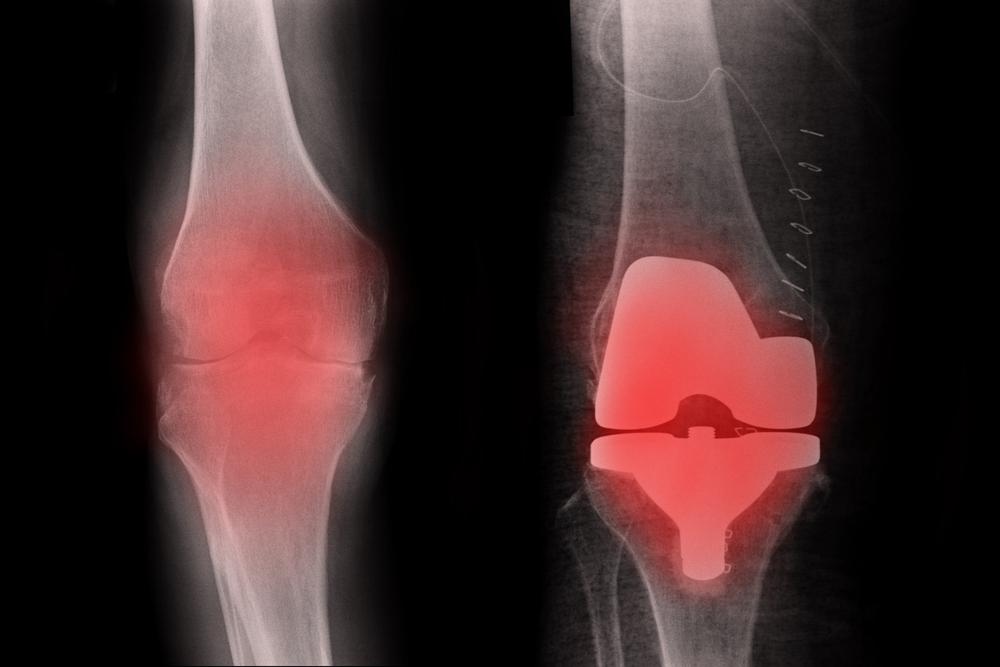
Several advances and changes in techniques are responsible for this dramatic shortening of the joint replacement experience. One caveat: The shortened process starts with healthy patients. Older people with significant health risks are still better off in a monitored hospital setting when undergoing any major surgery.
But most arthritic patients are healthy, with just a painful joint. For them, the process begins with patient education. This includes preoperative physical therapy (to maximize the range of motion of the joint) and learning rehabilitation exercises, as well as crutch and cold compression therapy device use. (The cold compression devices significantly reduce post-operative pain and swelling.) Of equal importance is a visit with the surgical nurse, to review in advance the choice and use of non-narcotic pain medications. These might include Ketorolac (Toradol), aspirin, Tylenol, Lidocaine patches and possibly a “rescue” narcotic for break-out pain or sleeping medication if necessary.
Eliminating the narcotics has been a primary factor in the reduction of complications. Narcotics not only make people nauseated; they decrease muscle function, cause urinary retention and slow recovery. Having the safest tools for pain reduction at home, and knowing how to use them, makes the first few nights after surgery far more pleasant than being in the hospital—awakened every few hours (or less) for vital signs or by hospital sounds.
A few key changes have been made during surgery as well. First, patient-specific cutting guides and customized implants, along with robotic or computer guidance, allows smaller surgical incisions. This translates to less cutting of nearby tissue, more precise placement of implants, and faster surgery. A new drug called tranexamic acid stops the bleeding locally, yet magically does not increase the risks of blood clots. This advance has eliminated the need for tourniquets, which produced significant post-op pain, and muscle and nerve compromise.
The use of large volumes of dilute Xylocaine (an anesthetic) -related drugs called Robivucaine or Marcaine, deposited in a pocket behind the knee capsule, causes the slow release of these compounds into the joint itself during the first 24 hours. Combined with cold compression, this strategy allows most total knee joint patients to leave the operating room pain-free—and stay that way—for 24 to 36 hours. A diligent schedule of additional non-narcotic pain relievers make the next few days quite manageable. And since the patients are in our physical therapy area each day for soft tissue massage and guided exercises, any break-out pain can be controlled immediately.
And this process benefits more than the patient. The cost savings to the medical establishment are also substantial. It is estimated that the average hospital cost for a total knee is nearly $60,000[1] dollars. Today there are 719,000[2] knee replacements performed each year; estimates suggest this will increase to 3.48 million total knees in 2030.Moving to outpatient care can cut these costs by two thirds, creating great savings for both patients and insurance companies.
The physical therapy part of the process is also critical. Daily physical therapy mobilizes the joint, reduces the swelling that inhibits healing, and encourages well-body exercises such as single-leg bicycling. Such exercises blow off the remaining anesthetics, and stimulate wellbeing.
Needless to say, there’s a strong psychological benefit to this as well. Starting the recovery program immediately, in an outpatient setting, makes patients feel like athletes in training—not patients in rehab. And who wants to be a patient in rehab, anyhow?
