Repair of Clavicle Fractures
The clavicle, or collarbone, is broken most frequently in falls—from bikes, while skiing, and when doing other sports. A twisted, thin, flat bone, the clavicle presents lots of problems for surgeons trying to fix fractures. Here are some of the pitfalls.
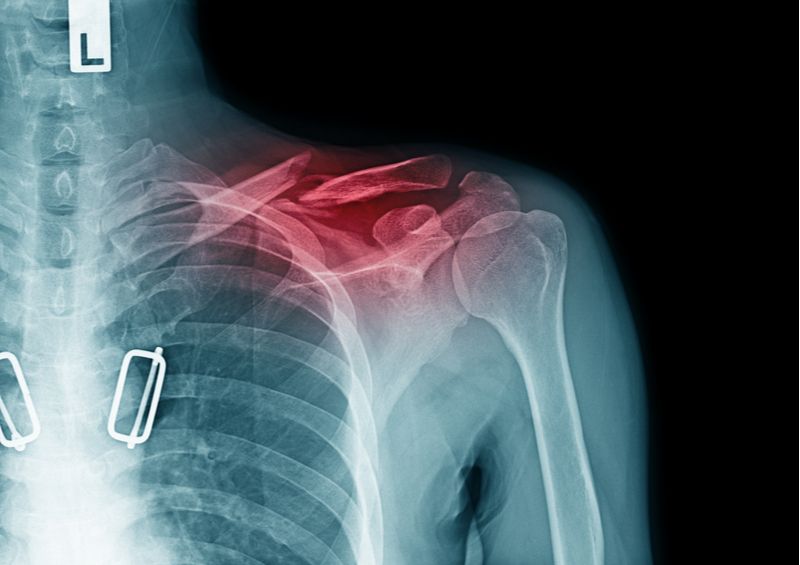
The clavicle acts as a strut, reaching from the sternum to the scapular of the shoulder. It can be fractured by a fall or a direct blow. I broke mine when I fell face first skiing—while I was working, ironically, as an orthopaedic surgeon for a ski race. The walkie-talkie radio strapped to my chest was driven straight through my clavicle. Classically, surgeons have had three choices: leave the bones to heal on their own, fix the pieces with a steel plate and multiple screws, or place a screw lengthwise down the barrel of the bone.
Left alone, simple fractures of the middle of the clavicle, without displacement, heal well without surgery—most of the time. Unfortunately, they don’t always heal fully; and if there is angulation of more than 45 degrees, or if the bone has multiple fractures, they frequently fail to heal at all. (Fractures near the very tip of the clavicle, next to the acromion, have their own set of issues, and usually need prompt repair.)
The repair of this twisted, thin bone, which contains very little marrow and rests directly under the skin (without much of a fat covering), has unique challenges. In addition to its tortuous anatomy, a superficial nerve runs right over the middle of the bone. If not protected during surgery, damage to this nerve can leave the patient with chest numbness.
The plates classically used for repair must be twisted and shaped to match the bone. Drilling multiple holes weakens the bone. Since people who break their clavicles are often very active, it is not recommended to leave the plates in after healing, as a new fracture with the hardware in place is even more complicated. For this reason, a second surgery to remove the plates and screws—usually after 6-12 months—is recommended.
These plates and screws also carry a risk of infection and malunion, or non-union, as the blood supply to the injured area is limited, and the skin coverage thin. These complications happen more often than we wish.
To overcome those weaknesses, we prefer to place a pin or screw down the barrel of the clavicle instead of the plate. The advantage is less surgical exposure, fewer holes in the bone, no plate under the thin skin, and immediate stability. The disadvantage is that it is often tricky to line up the curved, twisted bone to accept a straight screw. Flexible screws have been designed to solve that part of the challenge, but they have not been as reliable as the straight ones.
Since any technique has the potential to fail, using procedures that are salvageable in a second surgery is one key to avoiding long-term problems. Taking advantage of up-to-date science is a way to avoid such problems in the first place.
With any of these repair techniques, we add growth factors. These recruit the body’s own stem-derived repair cells to accelerate healing. We want to win the race between complete healing and our patients’ chance of reinjuring themselves.
It’s often a close contest. As my patient who competed in the bike Race Across America (RAM) 10 days after his clavicle fracture was pinned said: “I am not pedaling with my arms….”
See how Dr. Stone performs clavicle fracture repairs percutaneously

