PCL Injuries: Never simple, and not to be ignored
The PCL (posterior cruciate ligament) can be ruptured in car accidents when the knee hits the dashboard and in ski accidents when knees get impacted in wild falls. If left alone, the injured knee degrades over time. Understanding the injury and novel ways to treat it has changed its natural history.
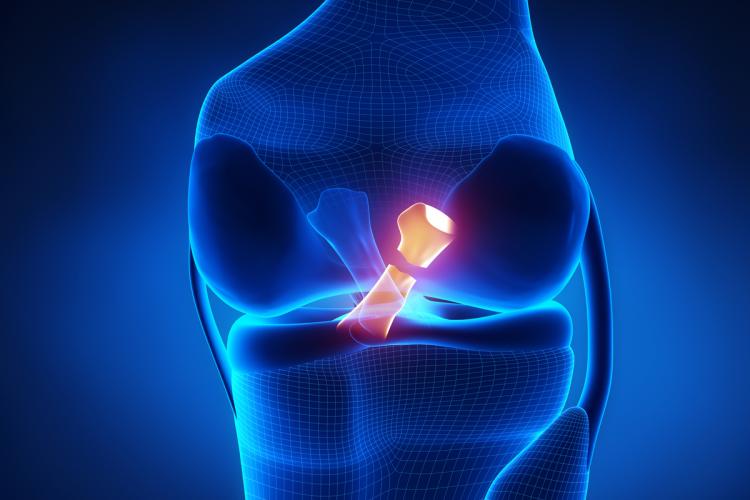
The posterior cruciate ligament extends from the back of the tibia to the front of the femur, inside the knee. It stops the tibia from going backwards when hit from the front and guides the rotation of the knee in synchrony with the ligaments that surround it. For years surgeons advised patients to live with their injured ligament, as repair or reconstruction were difficult and the disability was not too bad. Yet over time those untreated knees degraded, arthritis set in, and knee replacements ensued.
Today we understand that the PCL can sometimes be repaired. This is done with sutures anchored to the bone (when partially torn) or reconstructed with donor tissues when completely ruptured. The best repairs and reconstructions are those done immediately after the injury when the tissues are fresh and the joint is not further stretched out. What is new is that the insertions of the PCL extend over such a wide area that it has become mandatory to use large tissue replacements to get an optimum result. The more collagen and the thicker the tissue used in these insertions, the better. And the sooner the better, as over time the PCL tissues scar down and the supporting structures become stretched out.
Our donor tissues are now pre-loaded with anabolic growth factors from both concentrated blood (PRP) and from amniotic tissues containing growth factors at the time of implantation. It is believed that by boosting the early healing response the thick replacement tissues may heal faster, though the definitive data is not yet in.
But it has also become clear that a PCL injury is rarely an isolated injury. To put enough force on the knee joint to rupture this key structure, other supporting ligaments and tissues often give way. We rarely see a torn PCL without an injury to the corners of the knee. These typically occur in the posterolateral corner which, if ignored, leaves the patient with only a partially functioning knee. Meniscus tissues are also frequently torn with the PCL and are best treated with an immediate suture repair. Left alone they become more degenerated and less repairable.
In sum, the knee joint works because a wide range of tissues collaborates to guide the joint through a complex series of rotations and flexion that describe normal knee motion. As we deepen our understanding of the relationships between the tissues, we appreciate how important it is to restore all of the supporting actors when the lead actor is obviously disabled. And once repaired—unless the tissues are then rehabilitated with exercises that stimulate normal maturation—scar tissue forms, degrading the final outcome.
There are no simple knee injuries that are big enough to tear a key guiding ligament. As our MRI imaging techniques improve and our mechanical testing becomes more refined, our surgical tasks will increase in complexity. Beware of the insurance companies and health care guidelines that limit repairs and restrict rehabilitation, that insist on generalist surgeons and not specialists, and that delay the time of injury repair. They may seem simple and cost-effective for the payer, but they doom the patient to an unnecessary lifetime of disabilities. Cost-effective for them is too often health-defective for you.
