Achilles Tears: The Debate Continues
Hear From Our Patients
Surfers Returns from Ruptured Achilles with Percutaneous RepairAchilles tendon ruptures are in the news. Season-ending, will take a year to come back, terrible injury…such verdicts fill the headlines. Why?
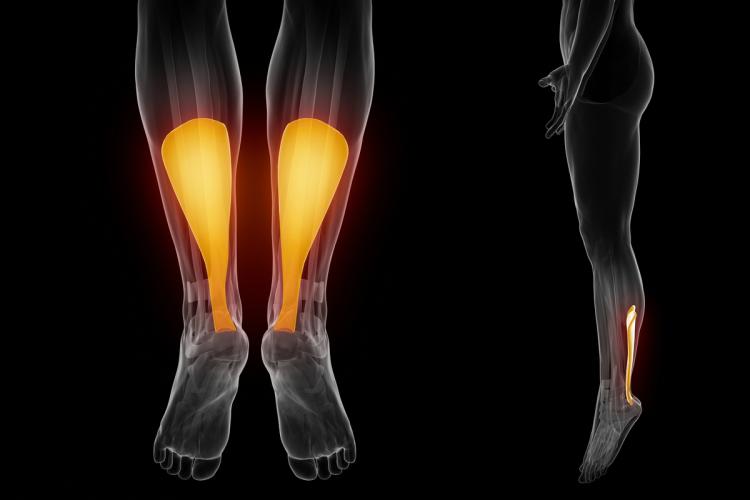
The Achilles tendon is a broad, strong, fibrous band connecting the calf muscles to the heel. It is designed to stretch and contract, which permits a forceful push off from the foot while walking. It ruptures most commonly in males over 50 when landing from a weekend basketball jump or lunging for an errant tennis ball. But it can also occur in elite athletes—like DeMarcus Cousins of the Warriors last year. In younger athletes and women, the tear is more commonly associated with the use of fluoroquinolone antibiotics such as Cipro (why this happens is unknown).
The debates usually revolve around whether or not to repair the tendon and whether to perform the repair open or by percutaneous closed surgical techniques. Here is our take.
None of our athletes choose non-operative healing. The reason is that, while the Achilles can potentially heal without surgery, the healing occurs with scar tissue filling in the rupture gap. This makes the tendon weaker. Few athletes want that outcome—or the risk of the tendon not healing at all.
We do not open the Achilles to repair it. When it ruptures, the sheath containing the tendon remains intact. The bleeding—with all of the progenitor cells and growth factors that blood brings—bathe the ruptured fiber ends. Many surgeons prefer the open technique so that they can see the ends of the tendon. But open surgery releases those healing factors, causes scarring of the sheath, and has not been demonstrated to be superior to the percutaneous technique.
The percutaneous technique, which we prefer, uses strong, absorbable sutures that we weave into the tissues through several small skin punctures. The ends of the ruptured tendon are pulled together, permitting healing at the tendon’s normal length. The sutures dissolve away and the tendon, sheath, and muscle tendon length all return to normal. We see no reason to use permanent sutures, devices, or other implants that increase the risk of infection or scarring.
The frustrating part, however, is that the healing takes so long. We try to accelerate the process by adding growth factors and progenitor cells. Yet while it makes sense to do this, we still don’t have the data to confirm that these interventions make a significant difference.
A second depressing factor is the degree of muscle atrophy we see in the calf during the healing time. The injury, the surgery itself, and the non-weight-bearing interval all conspire to weaken the calf muscles. While we try to exercise the quad and hamstrings—using stretch cords and other devices that isolate these muscle while not loading the calf muscles themselves—the leg weakness is still significant. There may be pharmaceutical interventions that could prevent some of this; however, they are still in the testing phase.
The Achilles tendon rupture remains a major injury with a slow recovery process. No wonder it is a feared event and a huge motivation for us to find better solutions.
Achilles’ mother didn’t understand anatomy. If you are going to be dipped into the river Styx, ask your mom to hold you by the big toe, not the heel.
What's the Best Way to Fix a Ruptured Achilles Tendon?
At The Stone Clinic, we repair Achilles tendon ruptures without open surgery using the Percutaneous Achilles Repair technique. Over the past 30 years, Kevin R. Stone, MD, has refined this approach to eliminate the need for a large incision, preserve growth factors that accelerate healing, and reduce infection risk. Here’s how.